LATERAL HIP PAIN
In recent years, we have termed the name Greater Trochanteric Pain Syndrome (GTPS) for any pathology involving the tendons of Gluteus Medius and Minimus and/or the Trochanteric Bursa. The gluteus medius and minimus are crucial for locomotion and mobility, as they provide lateral stability of the hip joint particularly when standing on one leg (Ganderton et al, 2019).
GTPS is a common complaint, particularly in women between 45-63 years old. It has been reported that the prevalence of unilateral GTPS was 15% for women and 6.6% for men, that is over 2x more common in women than men (Segal et al, 2007).
Symptoms of GTPS include:
- Intermittent or constant pain at or around the greater trochanter (lateral hip).
- Increased pain while sitting, stair climbing, walking, and lying on the affected side.
How is GTPS diagnosed?
Diagnosis of GTPS can be done by your physiotherapist. They will perform a battery of tests on your hip to determine the likely source of your pain. If there is any uncertainty of your diagnosis your physiotherapist may send you for further investigations (X-ray, MRI, U/S) to rule in or out other pathology.
Why does GTPS occur? What might lead to developing lateral hip pain?
It is normal for the Gluteus medius and minimus to atrophy (decreased in size) and dysfunction with healthy ageing. Degeneration of the gluteus minimus in particular has been associated with an increased risk of falls. Additionally, a reduction in estrogen in perimenopausal and post-menopausal women further increases the deterioration in muscles and tendons. There is increased evidence showing heightened tendon abnormalities, tendon thickening and declining muscle strength in this group (Ganderton et al, 2019). Overall, this results in a reduction of the capacity of muscles and tendons to tolerate increases in load.
Tendinopathy is most often the result of a rapid increase in load. In the case of the gluteal musculature this load may be compressive in nature, that is added pressure to the tendon such as lying on your side for prolonged or extended periods. Or it may be just a rapid increase in functional loading such as increasing the number of steps you are taking in your day, or hiking up a mountain when your body is not conditioned to it. These are just some examples of why GTPS may present.
What can I do to reduce my pain and help reduce the load on my gluteal tendons?
Below are some simple modifications you can make in your day to day activity to reduce the compression on your gluteal tendons which will commonly reduce your symptoms of GTPS.
- Reduce climbing stairs, walking up hills, and hip adduction across midline.
- Avoid sitting with legs or ankles crossed or hips positioned higher than knees.
- Equal weight-bearing through lower limbs when standing – no shifting to one side.
- Avoid side lying on affected side, if lying on opposite side – position a pillow between knees to keep legs in a more neutral position (Ganderton et al, 2018).
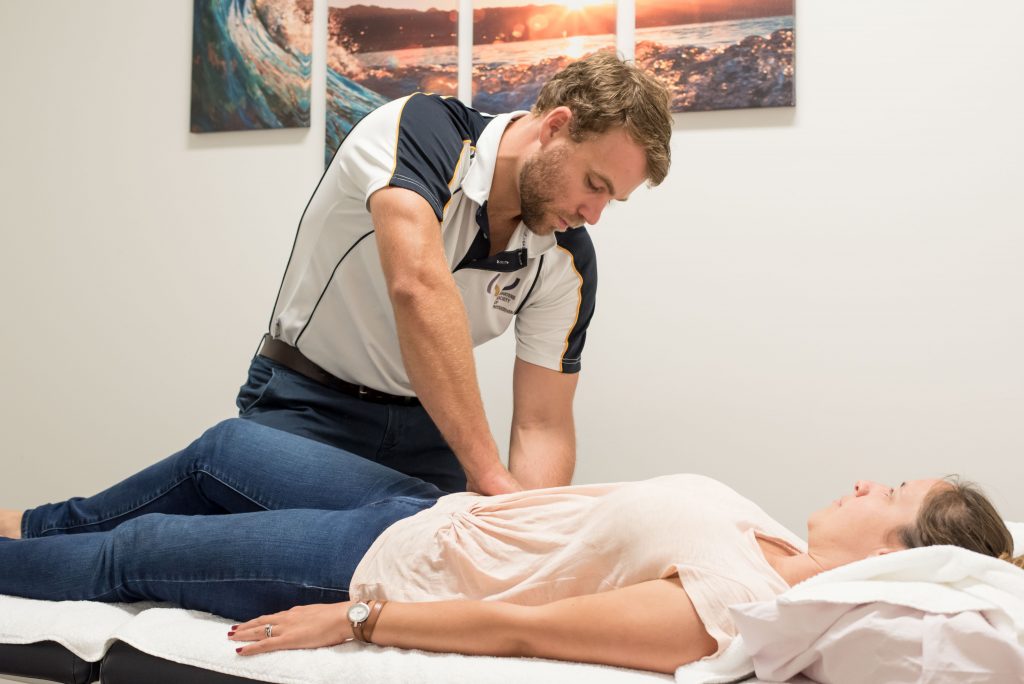 What can physiotherapy do for GTPS?
What can physiotherapy do for GTPS?
Initial aims of physiotherapy are to assist in pain reduction and getting you back to appropriate loading as soon as possible. Your physiotherapist will educate you on load management and individualise a program specific to you and your function depending on what your goals are. They will commonly perform muscular release techniques such as massage and dry needling to reduce the trigger points or tightness in the musculature surrounding your hip, this may help alleviate some of your pain and allow you to function better. They will then work with you to develop a gradual strength program for your hip and other lower limb musculature.
There has been new research conducted in perimenopausal and post-menopausal women to determine what exercises activate the gluteus medius and minimus musculature most effectively. Researchers compared seven common gluteal strengthening exercises and determined that the highest muscle activation was elicited in all portions of glute med and min with the hip hitch exercise. This research allows physiotherapists to be more accurate with their exercise prescription and progressions (Ganderton et al, 2019).
What other treatment may be recommended for GTPS?
Injections are commonly recommended to patients with GTPS – most commonly into the trochanteric bursa. Evidence has shown that corticosteroid injection and shock wave therapy have a greater reduction in pain at one month follow up, but at 15 months follow up, exercise therapy was much more beneficial to the pain and function of patients. In summary, corticosteroid injections may have a short-term effect on pain reduction but do not have the long-term benefits that exercise therapy will bring (Rompe et al, 2009).
References
Ganderton C, Semciw A, Cook J, Moreira E, Pizzari T. Gluteal Loading Versus Sham Exercises to Improve Pain and Dysfunction in Postmenopausal Women with Greater Trochanteric Pain Syndrome: A Randomized Controlled Trial. Journal of Womens’s Health. 2018.
Rompe JD, Segal NA, Cacchio A, Furia JP, Morral A, Maffulli N. Home training, local corticosteroid injection, or radial shock wave therapy for greater trochanter pain syn-drome. Am J Sports Med 2009;37:1981–1990.
Ganderton C, Pizzari T, Cook J, Semciw A. Gluteus Minimus and Gluteus Medius Muscle Activity During Common Rehabilitation Exercises in Healthy Postmenopausal Women. Journal of Orthopedics and Sports Physical Therapy. 2019.
Segal NA, Felson DT, Torner JC, Zhu Y, Curtis JR, Niu J, Nevitt MC. Greater trochanteric pain syndrome: epidemiology and associated factors. Archives of Physical Medicine and Rehabilitation, 2007;88(8):988-92.

