MENISCUS INJURY
The meniscus is a fibrocartilage structure that sits in the knee joint between the thigh bone and the shin bone. Its primary purpose is to be a shock absorber and stabiliser in your knee oint protecting the bone surfaces when you walk, run, jump, land and pivot. The meniscus in your knee joint is made up of two wedge shaped structures which we refer to as the medial (inner side of knee) and lateral (outer side of knee) meniscus (Doral et al, 2018).
 A meniscus tear occurs either traumatically or from gradual degeneration. Most commonly, traumatic tears occur when you twist on a bent knee. This is common when playing change of direction or pivoting sports. Degenerative tears occur more commonly in older adults due to natural age-related wear and tear.
A meniscus tear occurs either traumatically or from gradual degeneration. Most commonly, traumatic tears occur when you twist on a bent knee. This is common when playing change of direction or pivoting sports. Degenerative tears occur more commonly in older adults due to natural age-related wear and tear.
Meniscus tears are classified into different types depending on the location and size of the tear. Once we are able to classify the type of tear we can then make an appropriate management plan.
Patients who sustain a meniscus tear may experience the following symptoms:
- Pain
- Swelling
- Limited range of movement in their knee
- Catching
- Locking (Doral et al, 2018)
Meniscus tears are treated in one of three ways.
- Non-operative (physiotherapy)
- Meniscectomy (removal of part of the meniscus)
- Meniscal repair
Selecting the correct treatment for your meniscus tear is individualised depending on multiple factors such as your age, past history of injury, the type of tear (size and location) and what level of function you want to return to (Mordecai et al, 2014).
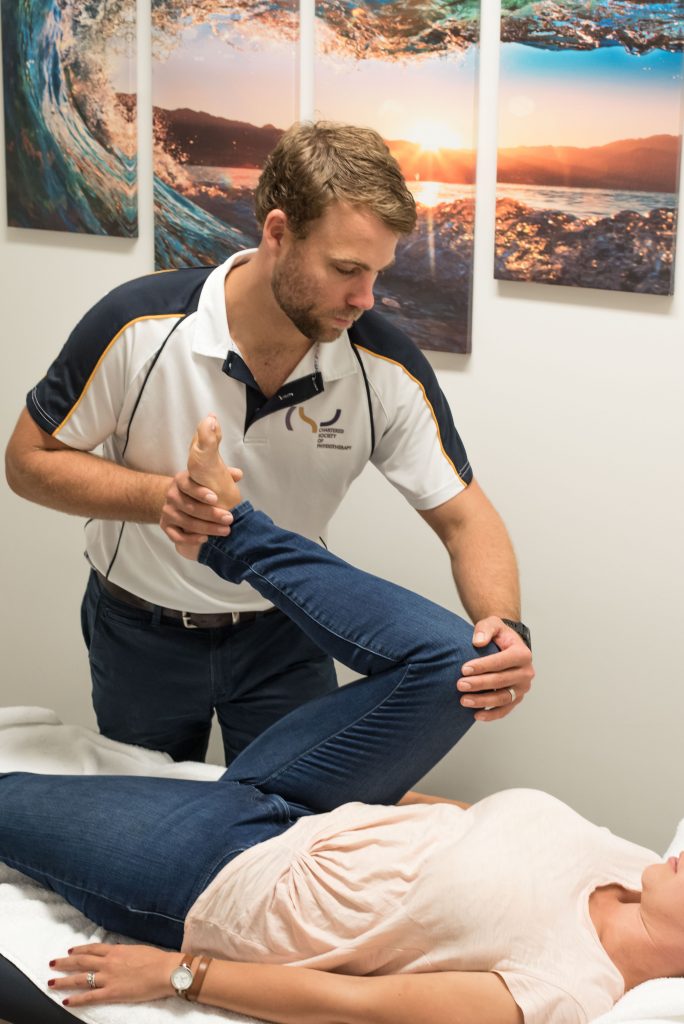 Treatment
Treatment
Physiotherapy should be considered as the first line of treatment for meniscus injury. At your initial consult with your physiotherapist they will conduct a number of tests to determine if it is likely you will be a surgical or non-surgical candidate. Sometimes you will require an MRI scan to determine exactly what type of meniscus injury you have sustained to give your physiotherapist a better understating of whether the tear is likely to heal on its own. There is strong evidence to suggest that degenerative tears without mechanical symptoms can be effectively treated non-operatively with structured physiotherapy (Mordecai et al, 2014).
Non-operative management with your physiotherapist involves at least three to six months of education, activity modification and most importantly strengthening exercises. In order for your physiotherapist to determine if non-operative management is going to be successful, patients must complete their strengthening exercises a minimum of twice a week for greater than 12 weeks (Doral et al, 2018).
A meniscectomy, as the name suggests, involves the surgical removal of part or all of the meniscus in your knee joint. Evidence has shown that removing the whole meniscus leads to an increase in the likelihood of osteoarthritis in the knee joint. Therefore, only the torn part of the meniscus is removed and as much of the meniscus is preserved at possible.
When is a meniscal repair required?
Considering the long-term complications associated with meniscectomy, and the clear functional importance of the meniscus, there has been increasing avoidance of meniscectomy and thus meniscal repair has gained popularity. Not all patients are suitable for meniscal repair. The blood supply to the area of the meniscus being repaired is fundamental to the success of a meniscal repair. It is well documented that only tears in certain zones (the red and red-white zone) are expected to heal. The lack of blood vessels in the remaining meniscus prevents healing in these zones.
Meniscal repair shows 80% success at two year follow up and is more suitable in younger patients with tears that are peripheral and horizontal or longitudinal in nature. However, having the surgery is not a sure fix, there are strict post-operative rehabilitation requirements including wearing a brace and not weight bearing for 4-6 weeks that must be followed to ensure the success of the repair (Mordecai et al, 2014). In addition to these post operative orders, patients will also be required to perform a progressive strengthening program with their physiotherapist.
Summary
Determining whether your meniscus tear requires surgery is dependent on multiple factors and is not always simple. Your physiotherapist will guide you down the right path to give you the most favourable outcomes.
Arthroscopic partial meniscectomy (APM) is one of the most common operations, with a steady increase in the number of these procedures performed from the 1990’s until the 2010’s. APM should be the last resort for most meniscal tears. Evidence has shown that at two years follow up patients with symptoms of degenerative medial meniscus tears have no added benefit to having APM. There is no evidence to support the idea that patients with presence of mechanical symptoms or certain types of meniscus tears are more likely to benefit from APM (Sihvonen et al, 2018). Surgery should not be the first line of treatment for patients with degenerative meniscus tears. It should only be considered after a minimum of three to six months of conservative management (Doral et al, 2018).
Research suggests that there is no significant difference in improvement in patients function five years after arthroscopic partial meniscectomy and supervised exercise when compared with supervised exercise alone. It is therefore recommended that a trial of supervised exercises is performed as a first line of treatment (Herrlin et al, 2013).

